For a patient with severe anaemia, the operating room is the ultimate challenge.
Their body is already fighting for oxygen before the surgery even begins. From a clinical perspective, ignoring low haemoglobin isn’t just a minor oversight; it is a major red flag for heart strain, slow healing, and post-op complications.
That is where preoperative anaemia management before gynaecological surgery becomes crucial. It acts as the bridge between a high-risk procedure and a safer, smoother recovery.
Through this blog, let’s explore why pre-surgical optimisation becomes important.
Why Severe Anaemia Makes Gynaecological Surgery Riskier?
Do you know what anaemia is?
Anaemia is a condition marked by a deficiency of healthy red blood cells or haemoglobin, reducing the blood’s capacity to carry oxygen to tissues.
During gynaecological surgery, the body needs adequate oxygen to heal and manage blood loss. Now, let’s know in detail about the risk factors:
Risk of Infection and Slow Healing
The body’s ability to heal post-surgery depends largely on the oxygen delivered by haemoglobin. In an anaemic state, tissues heal more slowly, increasing the likelihood of wound infections, dehiscence (wounds opening), and other complications.
Women with low haemoglobin before surgery experience longer hospital stays, a higher chance of post-op infection, and prolonged recovery periods.
Anaemia existing before elective surgery is, in the majority of cases, of mild to moderate severity and can be diagnosed in up to 80% of patients, depending on the underlying disease. (Source)
The “Bleeding-Risk Combo” in Gynaecological Procedures
Surgical procedures like myomectomy (removal of fibroids) or hysterectomy (removal of the uterus) often come with a significant amount of blood loss.
If a patient has fibroids, the bleeding may have caused the anaemia in the first place. It is a vicious cycle: the fibroids cause heavy bleeding, and the surgery designed to remove them can lead to further blood loss.
This is exactly where addressing anaemia due to fibroids’ heavy bleeding treatment before surgery becomes critical. Optimising haemoglobin levels before the procedure helps break this cycle and makes the surgery significantly safer.
The Role of Patient Blood Management (PBM)
Patient blood management (PBM)in surgery anemia optimization is now considered essential in modern surgical care.
Instead of relying solely on transfusions during surgery, PBM strategies optimise a patient’s own blood reserves through iron supplementation and other means well in advance. This ensures the body is better prepared for surgery, reducing risks and improving outcomes.
Common Causes of Anaemia in Women Requiring Gynaecological Surgery

Anaemia in women can be caused by various gynaecological and non-gynaecological factors. Understanding these causes is crucial for managing iron levels and ensuring a safe surgery.
Fibroids and Abnormal Uterine Bleeding
The primary cause of anaemia for many women requiring gynaecological surgery is fibroids. These non-cancerous growths on the uterus lead to excessive bleeding during menstruation, causing a significant drain on the body’s iron levels.
Dr Smita Jadhav, a gyne surgeon in Salt Lake, can provide medical management to control bleeding and stabilise iron levels before surgery, making the procedure much safer.
Endometriosis and Adenomyosis
These conditions involve the lining of the uterus growing outside its normal area (endometriosis) or within the uterine muscle wall (adenomyosis). Both conditions often lead to chronic bleeding, which can cause significant iron loss over time. Optimising iron levels before surgery is critical to ensuring a smoother recovery.
Other Causes of Anaemia
In some cases, anaemia may be due to non-gynaecological causes such as:
- Vitamin B12 or Folate Deficiency: Common in vegetarians and those with poor nutrition.
- Thyroid Dysfunction: Can impact red blood cell production.
- Chronic Kidney Disease: Impacts red blood cell production and iron metabolism.
What Counts as Severe Anaemia Before Surgery?
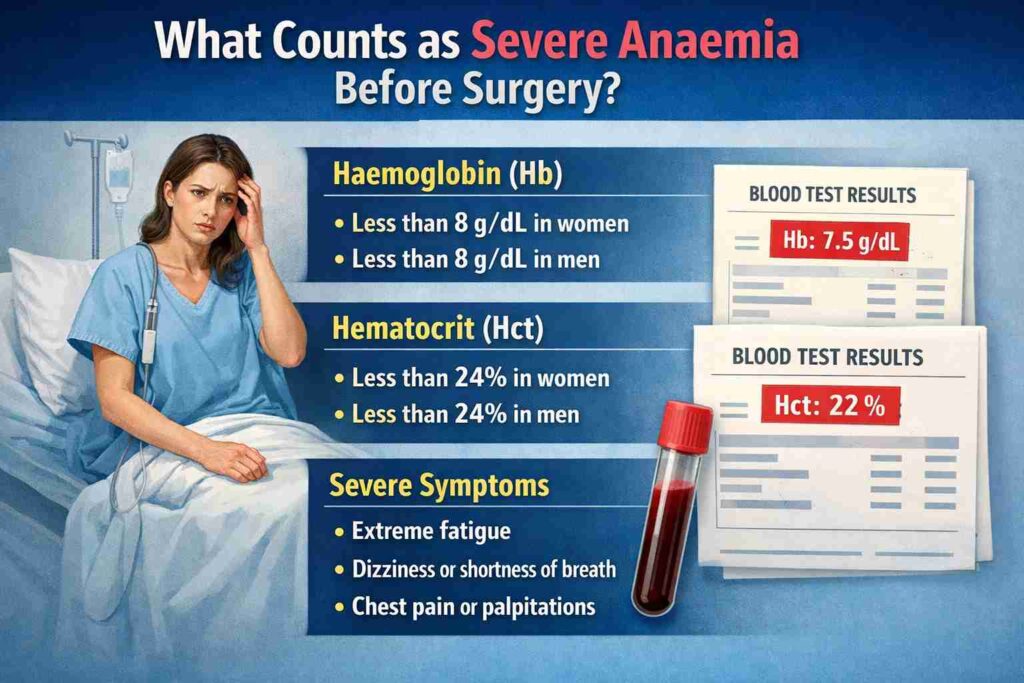
When preparing for surgery, particularly gynaecological procedures, understanding your haemoglobin levels is essential. Anaemia, especially severe anaemia, can significantly complicate the surgical process.
Identifying the severity of anaemia before the procedure is the first step toward optimising your health and ensuring a smoother surgical experience.
Severe anaemia before hysterectomy: What to do
Severe anaemia should be corrected before surgery to reduce risks. Doctors may delay the procedure and start iron supplements, IV iron, or blood transfusions if needed.
Treating the underlying cause and monitoring haemoglobin levels help ensure a safer hysterectomy and a smoother recovery.
Haemoglobin Levels: The Standard for Anaesthesia and Surgery
For surgical procedures, a haemoglobin level below 7-8 g/dL is classified as severe anaemia. Even a more moderate anaemia level (9-10 g/dL) presents risks, as it makes anaesthesia and blood loss during surgery far more dangerous.
When the body is already oxygen-deprived before surgery, the risk of complications increases significantly. In particular, there’s a higher likelihood of needing ICU care or longer hospital stays due to oxygen deprivation and slower healing.
The Symptoms That Should Trigger Pre-Op Testing
If you are anaemic, there are signs that demand further testing before surgery:
- Chronic Fatigue: Feeling exhausted no matter how much you rest.
- Breathlessness: Shortness of breath with simple activities like walking or climbing stairs.
- Dizziness: Feeling lightheaded or experiencing cravings for non-food substances like ice or clay.
If any of these symptoms sound familiar, it is essential to get a blood test and ensure your haemoglobin levels are within a safe rangefor surgery.
The Pre-Surgery Anaemia Test
Before surgery, your gynaecologist will order several tests to assess your anaemia and plan for optimisation.
These include:
| Test | Purpose |
| CBC + Indices | Measures haemoglobin levels and cell size (MCV). |
| Ferritin & Iron Studies | Evaluates iron stores in the body, not just circulating iron. |
| CRP (C-Reactive Protein) | Measures inflammation that could hinder iron absorption. |
| B12/Folate | To check for nutritional deficiencies, particularly in those on vegetarian diets. |
How to Increase Haemoglobin Fast Before Surgery
Think of your haemoglobin as your body’s internal battery life for surgery; you want to hit that ‘100%’ mark before you go under. Surgery is a marathon for your tissues, and since iron carries the oxygen needed for healing, loading up now is like fast-charging your system.
Focus on iron-rich fuel and Vitamin C ‘boosters’ to make sure you wake up with your recovery engines already revving.
Here are practical ways to raise your haemoglobin levels before surgery:
- Oral Iron Supplements
If your surgery is weeks away, taking iron supplements is an effective way to boost your levels. However, it can take time, and some women experience digestive discomfort with oral iron.
- IV Iron Infusion
For quicker results, IV iron therapy is the most effective solution. It bypasses the digestive system and delivers iron directly to the bone marrow, which can significantly raise haemoglobin levels in just 1–2 weeks. This method is preferred for women who need to optimise their levels quickly before surgery.
- Hormonal Control
If heavy menstrual bleeding is the cause of your anaemia, doctors can prescribe medications to help control the bleeding while you build your iron levels.
- Blood Transfusion
While not the first choice, a blood transfusion can be used in emergencies where haemoglobin is critically low, typically below 6–7 g/dL.
Post-Surgery Care: Continuing Blood Management
After surgery, the focus shifts to rebuilding iron stores. Despite successful surgery, your iron reserves will remain depleted, and it’s important to continue iron supplementation for 3–6 months post-op.
Questions to Ask Your Gynaecologist with Expected Answer
- “What haemoglobin level should we aim for before surgery?”
Expected Answer: The ideal haemoglobin level before surgery is typically around 12-15 g/dL, depending on the patient’s condition and the type of surgery.
- “Do I need ferritin or iron studies in addition to a CBC?”
Expected Answer: Yes, ferritin and iron studies may help assess iron stores, especially if anaemia is present.
- “Can we use medications to control bleeding before the surgery?”
Expected Answer: Yes, medications such as tranexamic acid or desmopressin can sometimes be used to control bleeding before surgery, depending on the patient’s needs.
The Role of Anaemia Management in Safe Surgery
Severe anaemia before gynaecological surgery significantly increases the risk of complications, including poor anaesthesia response, excessive blood loss, and delayed healing.
Pre-surgical optimisation, such as iron supplementation, is critical to improve oxygen levels and ensure a safer procedure. Managing anaemia before surgery is essential for minimising risks and promoting a smoother recovery.
To book an appointment with Dr Smita Jadhav, a gyne surgeon in Salt Lake, call +91 9748825624 today.
People Also Ask
Can surgery be postponed to treat anaemia first?
Yes, surgery can be postponed for 1–2 weeks to raise haemoglobin levels, ensuring the patient is in better condition for the procedure.
Is IV iron safe?
Yes, modern IV iron formulations are generally very safe, with a significantly lower risk of adverse reactions than older formulations.
Can anaemia return after a hysterectomy?
If the anaemia was caused by uterine bleeding, it is usually resolved permanently after the hysterectomy. However, maintaining a healthy diet to replenish iron stores is crucial.